Digital Health Revolution: How Telemedicine and AI Are Transforming India’s Healthcare Delivery in 2026
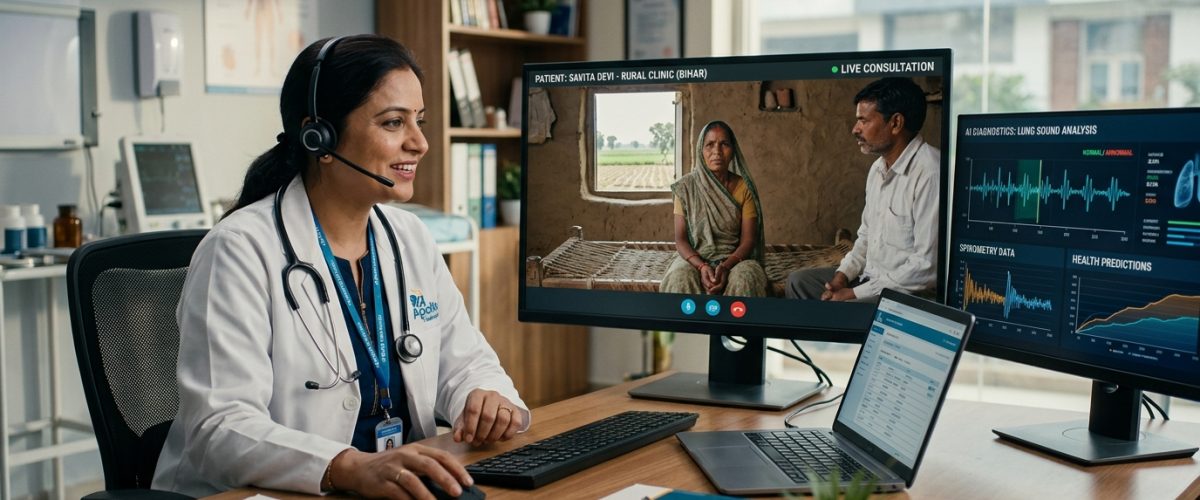
A Healthcare System in Digital Transformation
India’s healthcare system—historically characterised by stark urban-rural disparities, chronic underfunding, and a shortage of trained professionals—is undergoing a digital transformation that promises to fundamentally alter how healthcare is accessed, delivered, and financed. In 2026, the convergence of telemedicine platforms, AI-powered diagnostics, digital health records, and mobile-first health applications is creating a parallel healthcare infrastructure that complements the physical hospital and clinic network. This digital layer, while still in its early stages, has the potential to extend quality healthcare access to hundreds of millions of Indians who have historically been underserved.
The scale of India’s healthcare challenge provides context for the digital health opportunity. India has approximately 1 doctor for every 1,000 people—below the WHO-recommended ratio of 1:1,000 and far below the ratios in developed nations. The distribution is even more skewed: urban areas have 5-6 times more doctors per capita than rural areas. A villager in eastern Uttar Pradesh or rural Jharkhand may need to travel 50 kilometres to reach a qualified physician, often losing a day’s wages in the process. Digital health technologies, accessed through the smartphones that now penetrate 65 per cent of Indian households, can bridge this access gap in ways that physical infrastructure expansion cannot match in speed or cost-effectiveness.
Telemedicine at Scale: Beyond the Pandemic Experiment
The COVID-19 pandemic compressed years of telemedicine adoption into months, but the real story of digital health in India begins after the pandemic, as the temporary necessity has evolved into permanent infrastructure. In 2026, an estimated 15 crore Indians have used telemedicine services at least once, with approximately 3 crore regular users. The market, valued at approximately $5 billion, is growing at 25-30 per cent annually, making India one of the fastest-growing telemedicine markets globally.
The telemedicine landscape in India features three distinct models. The platform model, exemplified by Practo and MediBuddy, connects patients with independent physicians through video and chat consultations. The hospital-integrated model, led by Apollo 24/7, Max Healthcare’s digital platform, and Manipal Hospitals’ online service, offers teleconsultations as an extension of the hospital experience, with seamless referral to in-person care when needed. The government model, operating through the eSanjeevani platform, has facilitated over 15 crore teleconsultations since its launch, primarily connecting patients in rural health centres with specialists in district and state hospitals.
The eSanjeevani platform deserves particular attention for its scale and social impact. Conceived as a component of the Ayushman Bharat programme, it operates on a hub-and-spoke model where healthcare workers at primary health centres initiate teleconsultations with specialists at tertiary hospitals. The platform has been especially effective for chronic disease management—diabetes, hypertension, and respiratory conditions—where regular monitoring and medication adjustments can be conducted remotely, reducing the need for physical hospital visits that are burdensome for rural patients.
AI Diagnostics: Bringing Specialist Expertise to Every Clinic
Perhaps the most transformative application of AI in Indian healthcare is in diagnostics, where machine learning algorithms are achieving specialist-level accuracy in interpreting medical images, pathology slides, and clinical data. The impact is most profound in areas where specialist shortages are most acute: radiology, pathology, ophthalmology, and dermatology.
In radiology, Indian startups including Qure.ai, DeepTek, and Predible Health have developed AI algorithms that can detect tuberculosis, pneumonia, lung cancer, and fractures from chest X-rays and CT scans with sensitivity and specificity exceeding 95 per cent. Qure.ai, which has been deployed in over 40 countries, is being used in Indian government hospitals to screen for TB—India bears the world’s highest TB burden—enabling earlier detection and treatment initiation in facilities that lack full-time radiologists. The broader implications for India’s AI capabilities were explored at the India AI Summit 2026, where healthcare applications featured prominently.
In ophthalmology, AI-powered retinal screening is addressing the challenge of diabetic retinopathy, which affects approximately 15-20 per cent of India’s 100 million diabetic patients. Companies like Forus Health (Bengaluru) and Remidio have developed portable fundus cameras with integrated AI that can screen for retinopathy at primary health centres, identifying patients who need referral to ophthalmologists before vision loss becomes irreversible. The cost of such screening—approximately ₹50-100 per patient—is a fraction of the economic burden of preventable blindness.
The Ayushman Bharat Digital Mission: Digital Infrastructure for 1.4 Billion
The Ayushman Bharat Digital Mission (ABDM), launched in 2021 and now reaching operational maturity, represents the most ambitious national digital health initiative globally. The mission’s core components—the ABHA (Ayushman Bharat Health Account) health ID, the Health Information Exchange and Consent Manager (HIE-CM), and the Health Professional Registry—create a federated digital health infrastructure that enables interoperability across India’s fragmented healthcare ecosystem.
As of March 2026, over 60 crore ABHA health IDs have been generated, and over 3 lakh healthcare facilities—including hospitals, clinics, diagnostic centres, and pharmacies—are registered on the network. The HIE-CM allows patients to control access to their health records, sharing them selectively with healthcare providers through a consent-based mechanism. This interoperability means that a patient treated at a government hospital in Tamil Nadu can share their medical history with a private specialist in Delhi with a simple consent approval on their smartphone.
For healthtech startups, ABDM provides a standardised integration layer that dramatically reduces the cost and complexity of building healthcare applications. Instead of negotiating individual integrations with hundreds of hospitals and diagnostic chains, startups can build on ABDM’s APIs to access a national network of healthcare providers and patient data (with consent). This infrastructure effect is analogous to UPI’s impact on fintech—by creating a shared digital foundation, the government has lowered barriers to innovation and competition.
Digital Therapeutics and Remote Patient Monitoring
Digital therapeutics (DTx)—evidence-based therapeutic interventions delivered through software applications—is an emerging category in Indian healthtech. Companies like Wellthy Therapeutics and BeatO are building diabetes management platforms that combine continuous glucose monitoring, AI-powered dietary and medication recommendations, and regular teleconsultations with endocrinologists. BeatO, which serves over 10 lakh diabetes patients, has demonstrated meaningful improvements in HbA1c levels (a key diabetes control metric) among its users, providing clinical evidence that digital intervention can complement traditional treatment.
Remote patient monitoring (RPM) is similarly gaining traction, particularly for post-surgical care and chronic disease management. Connected devices—blood pressure monitors, pulse oximeters, glucometers, and ECG patches—that transmit data to healthcare providers via mobile apps are enabling continuous care models that were previously possible only in hospital settings. The cost of such devices has fallen dramatically, with connected glucometers now available for under ₹1,500 and connected blood pressure monitors for under ₹2,000, making RPM accessible to India’s expanding middle class.
Challenges and the Path Forward
Despite remarkable progress, India’s digital health transformation faces significant challenges. Data privacy and security concerns loom large as millions of sensitive health records move to digital platforms. The Personal Data Protection Act, enacted in 2023, provides a legal framework, but implementation and enforcement remain uneven across the healthcare sector. Cybersecurity incidents involving health data—including a notable breach at a major hospital chain in late 2025—have highlighted the vulnerability of digital health systems.
The interoperability challenge, while addressed at the infrastructure level by ABDM, remains practically limited. Many private hospitals and diagnostic chains have been slow to integrate with ABDM, citing concerns about data sharing, competitive advantage, and implementation costs. Achieving true interoperability—where a patient’s complete medical history flows seamlessly across providers—will require both regulatory mandate and economic incentives that make participation more attractive than isolation.
As India’s broader economy accelerates, supported by developments like the RBI’s optimistic GDP forecast and investment trends reflected in venture capital’s return to Indian startups, the healthtech sector has the resources and momentum to address these challenges. The goal is nothing less than building a healthcare system that leverages technology to deliver equitable, quality care to every Indian—a goal that is ambitious but, for the first time, technologically achievable.
- India Power Demand Shatters All Records at 265 GW as Deadly Heatwave Pushes Temperatures Past 48 Degrees Celsius Across Northern India - May 30, 2026
- SpaceX Files for Largest IPO in History at 1.75 Trillion Dollar Valuation as Starlink Revenue Soars to 11.4 Billion - May 30, 2026
- Magnus Carlsen Beats World Champion Gukesh in Norway Chess Round 4 — Bounces Back After Painful Losses to Climb Standings - May 29, 2026


